Adhesive Capsulitis (Frozen Shoulder): Causes, Symptoms & Treatment Options. Do You Have A Question? Speak To A Therapist Today. Call (24/7): 1300-003-777.
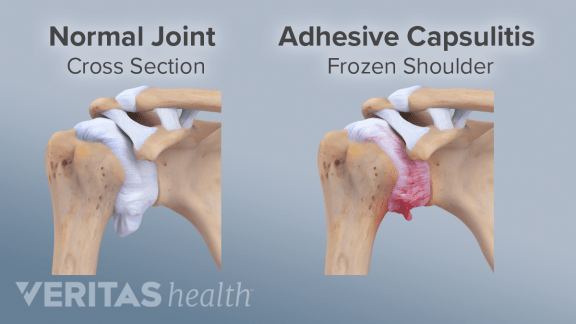
Adhesive Capsulitis (also called Frozen Shoulder) is a condition affecting the shoulder. The shoulder becomes painful, stiff and difficult to move. It’s currently thought that Capsulitis Shoulder has an unknown cause but clinical presentation demonstrates a person who has significant reduction in both passive and active shoulder movement. Imaging of the shoulder joint usually shows no abnormality. Many problems of the shoulder effect active range of motion however the obvious loss of passive range of motion is considered a hallmark feature of Frozen Shoulder Syndrome. Frozen shoulder symptoms are divided into three phases:
- FREEZING (PAINFUL): The initial phase is marked by a gradual onset of shoulder pain that may persist for weeks to months.
- FROZEN (STIFFENING): Characterized by a progressive loss in shoulder movement.
- THAWING: Demonstrates slow but gradual improvement in movement and reduction of shoulder pain.
Adhesive Capsulitis Epidemiology
The exact reason why some people experience Frozen Shoulder remains unknown. The condition is classified as either primary or secondary. Adhesive Capsulitis is considered primary if the onset is idiopathic (unknown) while secondary is classified when there is an obvious cause. Classic presentation of the deformity is an individual between the ages of forty to sixty years, with more females then males affected. It’s estimated that between 2 – 5% of people will suffer from the injury during their lifetime. Capsulitis of the shoulder rarely occurs in both arms. Diabetes Mellitus has been identified as a major risk factor with Diabetics being up to five times more likely to develop symptoms.
Conditions Which Mimic Adhesive Capsulitis
- SHOULDER JOINT OSTEOARTHRITIS: Loss of shoulder movement and pain will be present. Shoulder joint radiography should be used to rule out Osteoarthritis.
- SHOULDER IMPINGEMENT SYNDROME: Affects the Supraspinatus tendon of the shoulder & causes pain during arm abduction. Other movement is usually normal.
- SHOULDER BURSITIS: The pain and stiffness between both conditions is similar. The major distinguishing feature is that movement is usually greater in Bursitis sufferers.
- ROTATOR CUFF INJURY: Individuals suffering from Rotator Cuff pathology may note reductions in range of motion and strength. Imaging will demonstrate abnormality.
- GLENOHUMERAL JOINT DISLOCATION: Usually occurs following direct trauma.
Physical Examination Of The Shoulder Region
Your practitioner may ask you to complete one of the following outcome measures:
- SHOULDER PAIN & DISABILITY INDEX
- DISABILITY OF ARM, SHOULDER & HAND SCALE
- VISUAL ANALOGUE SCALE
- SF-36
A typical shoulder region physical examination may include (but is not limited to):
- OBSERVATION for potential scapula winging, deformity, unlevelving of the shoulders and general posture.
- RANGE OF MOTION assessment of the shoulder, cervical and thoracic spine to determine the extent of limited movement.
- MUSCLE STRENGTHEN TESTING to assess surrounding muscles of the shoulder joint to ascertain if muscle weakness is apparent.
- NEUROLOGICAL & ORTHOPAEDIC EXAMINATION of your dermatomes, myotomes and reflexes to rule of potential serious pathology involving the cervical spine and associated structures.
Frozen Shoulder Treatment Options
Adhesive Capsulitis is a self-limiting condition but it may take many years for people to notice improvement. Sufferers can address pain, loss of movement and general function through manual therapy. Your treatment should consist of physical therapy, anti-inflammatory measures and exercise.
Chiropractic & Physiotherapy
Physical therapy such as provided by Chiropractors & Physiotherapist’s assist individuals with improving range of motion, reducing pain and therefore improving quality of life. Treatment that may be administered by such professionals may include:
- Mobilization of the cervical and thoracic spine and shoulder girdle complex
- Soft tissue massage to the shoulder structures to assist with pain reduction and mobility
- Postural exercise advice to assist with scapular and shoulder stability
- Physiological therapeutics such as Ultrasound, Shockwave therapy and low level laser treatment to assist with reducing inflammation
Corticosteroid Injections
Chiropractor Adhesive Capsulitis Research
- Individuals suffering from Adhesive Capsulitis (Frozen Shoulder) demonstrated greater improvement following high-grade shoulder mobilization techniques compared to low-grade mobilization techniques. Vermeulen, H. (2006). Comparison of high-grade and low-grade mobilization techniques in the management of Adhesive Capsulitis of the shoulder: Randomized controlled trial. Physical Therapy, 86(3); 355 – 368.
- Majority of patients presenting with Adhesive Capsulitis demonstrated clinically significant improvement following Chiropractic management consisting of cervical, thoracic and shoulder joint manipulative therapy. Murphy, F. et al., (2012). Chiropractic management of frozen shoulder syndrome using a novel technique: a retrospective case series of 50 patients. The Journal of Chiropractic Medicine, 11(4); 267 – 272.
Additional Information
If you wish to continue your reading about Adhesive Capsulitis then please click here.
